Advocating for our Pulmonary Fibrosis Community
Team Telomere attended the Pulmonary Fibrosis Foundation Summit, where leaders in pulmonary medicine, genetics, and patient advocacy gathered to discuss the care for people living with interstitial lung disease and pulmonary fibrosis (PF). Throughout the meeting, genetics and telomere biology emerged as central themes. Our team participated in key scientific and patient-facing sessions, contributed the Telomere Biology Disorder (TBD) community perspective, and emphasized the urgent need to make genetic and telomere length testing accessible as part of routine PF care.
Genetics and genetic testing: A new standard of care
One of the most relevant sessions for our community was “Genetics and Genetic Testing: A New Standard of Care.” The session was chaired by Dr. Joyce Lee and Dr. Chad Newton, with presentations from Dr. Newton, Dr. Jeremy Katzen, and genetic counselor Janet Talbert. Speakers reviewed what we currently know about the genetic causes of ILD/PF, how genetics can inform treatment decisions, and what modern genetic testing looks like in clinical practice.
A major focus was how genetic information can change care. In the PF space, genetics can explain why disease behaves differently from person to person, predict treatment response and tolerability, identify patients at higher risk of complications, and optimize lung transplant. They cited specific examples, including that immunosuppression may need to be adjusted in patients with very short telomeres. Speakers also discussed examples from published studies, including the PANTHER-IPF trial and the PRECISIONS clinical trial, highlighting how precision medicine approaches are becoming increasingly important.
Panelists shared personal algorithms on when to consider genetic testing. Genetic testing in PF is critical as it can directly change medical management, help clarify future risk, identify health issues outside the lungs, and provide useful information for relatives.
Team Telomere representatives, including Katie Stevens and Dr. Chris Reilly, addressed the room, sharing the clear importance of testing as well as the challenges the community faces in accessing testing and coordinated care. Katie shared, “it is like watching you all walk through mud,” underscoring how slow the pulmonary field has been to change despite strong scientific evidence and successful models in other specialties, such as hematology.
Is it in your DNA? Understanding genetics and familial pulmonary fibrosis
This session was designed specifically for people living with pulmonary fibrosis, their families, and caregivers. Led by Dr. Joyce Lee with speakers Dr. Chad Newton, genetic counselor Jennie Vagher, and Dr. Bess Flashner, the session focused on pulmonary fibrosis in the families, what genetic testing can tell us, and how families can use this information to make informed decisions.
The speakers explained how genetics contribute to disease risk. They discussed the difference between rare genetic changes that have a large effect and common genetic variations that each have small effects but can still add up. They discussed a key study, which showed that even relatives who feel completely well can already have early lung changes: when CT scans were done in symptom-free relatives of PF patients, about 36% showed early abnormalities. This highlighted why identifying familial disease matters.
The session then walked through how genetic results can help refine the diagnosis, determine who needs closer lung monitoring, guide screening of other organs, inform transplant planning and medication choices, and identify blood relatives who may benefit from testing or surveillance.
One speaker also discussed the “pros and cons” of genetic testing. Team Telomere helped powerfully reshape the conversation. To each of the points given, Team Telomere helped reshape the conversation responding with community experience, updated evidence, and solutions:
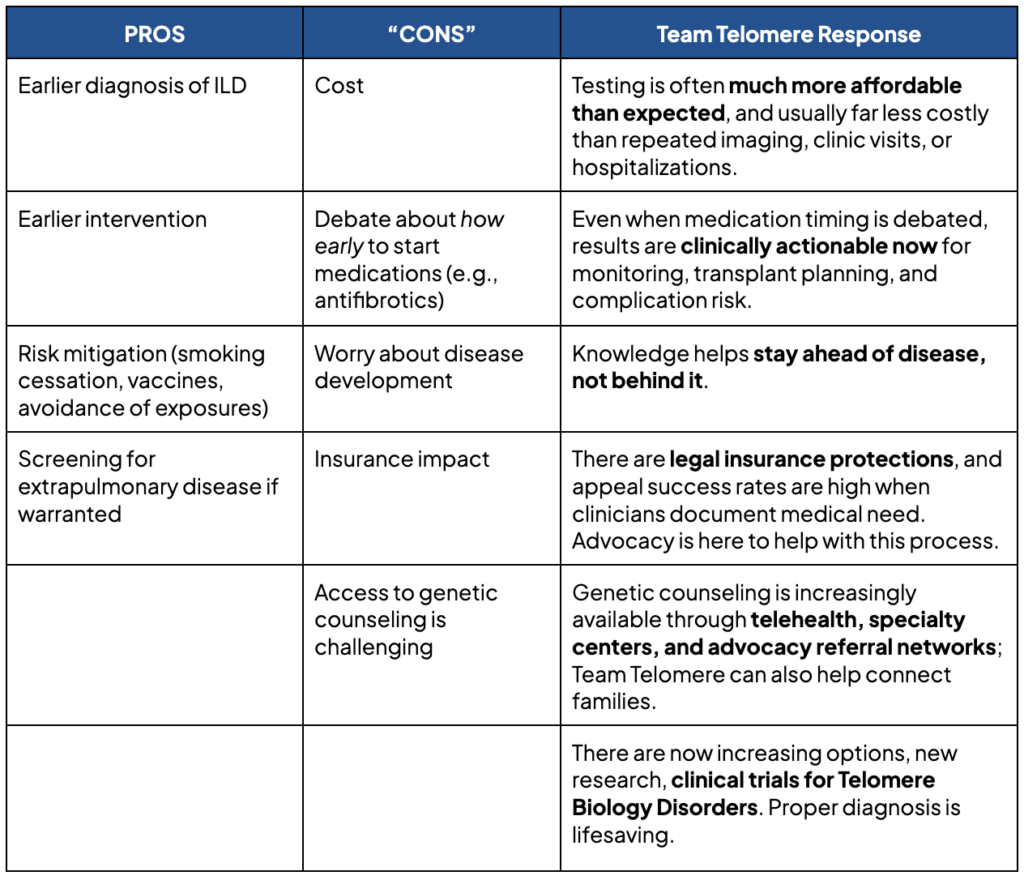
When audience members were asked whether they would pursue telomere length and genetic testing if cost and ordering barriers disappeared, nearly every hand in the room went up. The patient community made it clear that they want this information to guide their care.
The research is clear. Genetics in the PF space is moving from experimental to expected in ILD/PF care, and telomere biology has an essential place in that discussion. Team Telomere shaped the conversations at this conference, advocating for patients and families to receive genetic and telomere length testing given its clinically-actionable implications, and will keep working until this becomes the standard of care.

